
Ankle Swollen: The Guide to Do’s and Don’ts
Ankle pain is a common complaint here in Singapore, and a swollen ankle can dampen our active lifestyles. It can slow you down, whether you’re

Ankle pain is a common complaint here in Singapore, and a swollen ankle can dampen our active lifestyles. It can slow you down, whether you’re

Are you suffering from a painful ankle injury? Anyone can suffer from an ankle fracture, especially active individuals. If you suspect you have a broken
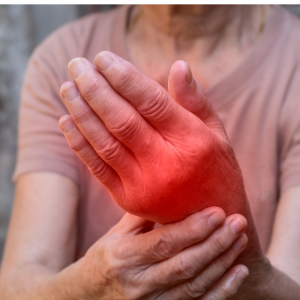
Understanding and Managing Gout Gout, a form of inflammatory arthritis, is a common and complex condition that can cause sudden and excruciating pain, swelling, and

Back Pain That May Be Serious Back pains—we’ve all felt it, grumbled about it, and maybe even popped a pain reliever or two for it.

Conquering Knee Pain Living in the vibrant city of Singapore, it’s easy to forget about your knees until they scream, “OUCH!” Knee pain can dampen
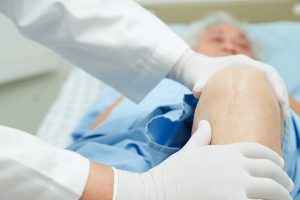
Knee Pain Post Op after Knee Surgery in Singapore: What to Expect and How to Cope Undergoing knee surgery in Singapore can be a significant

Join us as we delve into groundbreaking advancements in knee treatment and effective health screening. Admission is free! Learn more…
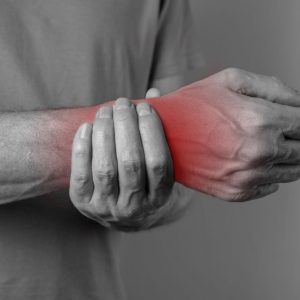
Struggling with chronic hand pain in Singapore? Discover advanced treatment options at Singapore Sports and Orthopaedic Clinic. Contact us today!

Have you ever experienced nagging discomfort in your neck that won’t let you be? Neck pain is more than an inconvenience; it can impact your
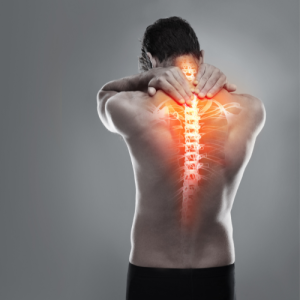
Lower Back Pain: Causes, Symptoms, Diagnosis, and Treatment This type of body pain can result from injuries, conditions, or diseases, most commonly affecting muscles or

Are You Having An Ankle Pain? Ankle pain refers to any discomfort or pain experienced in the ankle region. It can occur for various reasons,
Treatment of Lumbar and Thoracic Spine Fracture Lumbar and thoracic spine fractures can be a severe and potentially life-changing injury, causing significant pain and limiting

Our clinic offers same day appointment, X-ray/MRI facilities, Insurance filing services and amenities like pharmacy store & wheelchair accessibility.
© Singapore SPORTS and Orthopaedic Clinic

