
Ankle Pain Management
Are You Having An Ankle Pain? Ankle pain refers to any discomfort or pain experienced in the ankle region. It can occur for various reasons,

Are You Having An Ankle Pain? Ankle pain refers to any discomfort or pain experienced in the ankle region. It can occur for various reasons,

What is Rheumatoid Arthritis? Rheumatoid arthritis (RA) is a chronic autoimmune disorder affecting joints. The body’s immune system mistakenly attacks the lining of the joints,

Ankle pain is a common injury with various causes. From a sprain to a sudden onset of a painful sensation, ankle pain hinders one in
For most of us walking or running (except for the elderly) is a given. We usually take it for granted. But at times, because of

Ankle Sprains & Foot injuries are a common occurrence that can result while playing your favourite sport or maybe from a fall you experienced climbing

Sprained ankles are one of the most common sports-related injuries obtained by people. Although a sprained ankle may not be a major injury, pain in

Suffering from ankle pain when you’re trying to move can lead to less movement on your part. When you’re trying to stay in shape, get
If you’ve ever had a sprained ankle you know just how painful they can be. Sometimes they can feel as if you’ve broken bones or
Another name for progressive flatfoot is Posterior Tibial Tendon Dysfunction. The posterior tibial tendon is found in the calf down to the inside of the
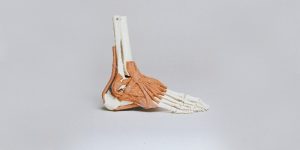
Our ankle joint is a complex structure involving bones, tendons and ligaments that helps to provide a wide range of motion including inversion, eversion, extension
Did you know that each person walks an average of 9000 steps per day? And the total distance covered by a person in his lifetime
Dancing is a physical activity that is accompanied with a certain level or risk. Dancing is something that needs to be gradually built up from

Our clinic offers same day appointment, X-ray/MRI facilities, Insurance filing services and amenities like pharmacy store & wheelchair accessibility.
© Singapore SPORTS and Orthopaedic Clinic

