
Ankle Pain Management
Are You Having An Ankle Pain? Ankle pain refers to any discomfort or pain experienced in the ankle region. It can occur for various reasons,

Are You Having An Ankle Pain? Ankle pain refers to any discomfort or pain experienced in the ankle region. It can occur for various reasons,

What is Rheumatoid Arthritis? Rheumatoid arthritis (RA) is a chronic autoimmune disorder affecting joints. The body’s immune system mistakenly attacks the lining of the joints,

Pain caused by arthritis can be quite uncomfortable, especially when it affects your finger joints. The symptoms of arthritis in fingers can make normal hand
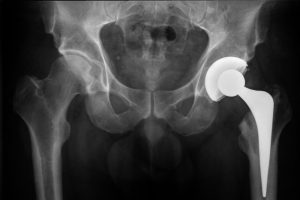
Our hips and knees undergo a lot of stress throughout our lives. These joints absorb substantial force and weight when we walk, jump, and move.

Ligament Tears are a common injury people experience, especially with those who are active in sports. Yet, many of us are quite clueless while trying
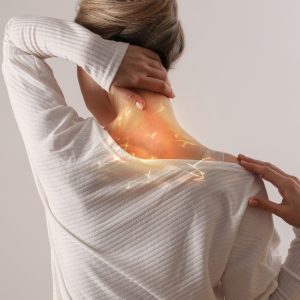
Have you ever woke up to a stiff neck before? That uncomfortable and tight feeling that makes movement almost impossible and causing you a lot
Osteoarthritis is a form of degenerative arthritis that causes pain and swelling in joints. Due to the wear and tear of cartilage in the joint,
The shoulder joint is composed of three different types of bones: the shoulder blade, upper arm bone and collarbone. This type of joint is a
Osteoarthritis is a degenerative disease that affects any joint in the body. One of the most common places is the hip due to the tremendous
Rheumatoid arthritis (RA) is not a selective disease. This indicates that RA can occur in any joint in the body, destroying it and causing pain
Total hip resurfacing arthroplasty is a surgical procedure with the intention of restoring the function of a hip for a patient suffering from degenerative joint
Immediately after your total joint replacement surgery, you will be moved into a recovery room to be monitored for a couple of hours. After the

Our clinic offers same day appointment, X-ray/MRI facilities, Insurance filing services and amenities like pharmacy store & wheelchair accessibility.
© Singapore SPORTS and Orthopaedic Clinic

