
Understanding and Treating Foot Pain
Get relief from foot pain with our orthopaedic specialists. Book an appointment for personalized treatment. Prioritize your mobility and well-being!

Get relief from foot pain with our orthopaedic specialists. Book an appointment for personalized treatment. Prioritize your mobility and well-being!

Are You Having An Ankle Pain? Ankle pain refers to any discomfort or pain experienced in the ankle region. It can occur for various reasons,

What is Rheumatoid Arthritis? Rheumatoid arthritis (RA) is a chronic autoimmune disorder affecting joints. The body’s immune system mistakenly attacks the lining of the joints,

Walking is the fundamental movement skill used in everyday activities, but overtime, it will lead to stress and pain of the feet, which are common

Ankle Sprains & Foot injuries are a common occurrence that can result while playing your favourite sport or maybe from a fall you experienced climbing
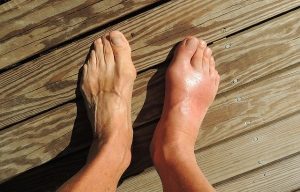
Looking for Orthopedic Bunion Corrector in Singapore? Let what Bunion Deformity Correction is first. Bunions & Bunionettes are a common cause of painful toes. A
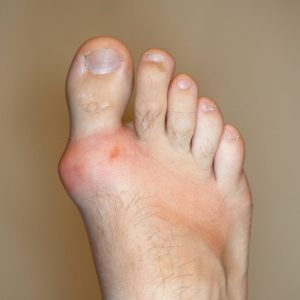
When it comes to everyday life your feet play a huge role. They take you from one place to the next, help you get where
Osteoarthritis is a form of degenerative arthritis that causes pain and swelling in joints. Due to the wear and tear of cartilage in the joint,
Hallux rigidus is a stiff big toe that occurs when there is an overgrowth at the base of the big toe. It prevents the toe
Tarsal coalition is a congenital condition that occurs when the tarsal bones at the back of the foot are abnormally connected, causing pain and limitations
Another name for progressive flatfoot is Posterior Tibial Tendon Dysfunction. The posterior tibial tendon is found in the calf down to the inside of the
Adult acquired flatfoot deformity (AAFD) is not present at birth and only acquired during adulthood between 40-60 years of age. Usually caused by damage to

Our clinic offers same day appointment, X-ray/MRI facilities, Insurance filing services and amenities like pharmacy store & wheelchair accessibility.
© Singapore SPORTS and Orthopaedic Clinic

